A peer-reviewed narrative review – “Integrative Role of Yoga and Naturopathy in Cancer Rehabilitation: A Narrative Review” – recently published in Cureus adds to the growing evidence base for yoga in oncology care — and raises important questions about what it will take to translate that evidence into standard practice.
Researchers at SDM College of Naturopathy and Yogic Sciences analyzed 13 studies published between 2000 and 2025, drawn from PubMed and Scopus, spanning breast, colorectal, lung, prostate, and hematologic cancer populations. They found that yoga interventions combining asanas, pranayama, and meditation showed consistent, clinically meaningful reductions across the symptom burden most common in people living with and beyond cancer.
Key findings include:
- Cancer-related fatigue – affecting 80% of people during or after treatment – showed moderate reductions sustained beyond the intervention period
- Anxiety and depression improved significantly
- Sleep disturbance, chronic pain, and physical dysfunction showed clinical benefit
- Quality of life improved across physical, emotional, social, and role functioning — with more pronounced effects in interventions lasting eight weeks or longer
The mechanistic data deserve particular attention. Yoga was associated with reductions in pro-inflammatory cytokines — IL-6, IL-1β, and TNF-α — alongside lower resting cortisol and improved heart rate variability. These are not peripheral markers. They are biological indicators directly linked to fatigue severity, immune resilience, and treatment tolerance.
Individualized Intervention: What the Research Requires
One of the review’s most practically useful contributions is its framework for matching yoga interventions to patient circumstances. The authors describe a clear continuum: chair or restorative yoga for those with advanced disease or limited mobility; gentle breathwork during or immediately after treatment; moderate Hatha or Iyengar-based practice for functionally recovered survivors; and online or hybrid formats for those managing geographic distance, immunocompromise, or mobility limitations.
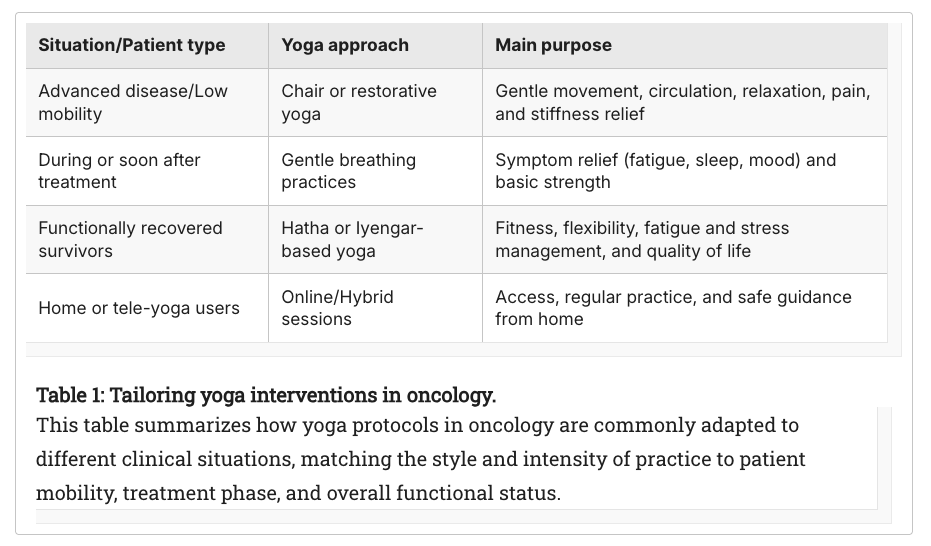
Individualized interventions is foundational to trained Oncology Yoga professionals. The support of this in peer-reviewed literature matters, because it reinforces a core principle: there is no single protocol for this population. Safe, effective Oncology Yoga requires individualized assessment, clinical knowledge of treatment side effects, and the judgment to adapt in real time.
The review is clear that outcomes are influenced by how interventions are delivered — and that working with this population requires practitioners who can evaluate disease stage, identify contraindications, and coordinate with the broader care team. That specificity distinguishes clinical Oncology Yoga from general wellness practice, and it reflects the case for specialized training.
The Barriers Are Real
The review’s forward-looking section addresses implementation honestly, and that honesty is worth reflecting.
The evidence now supports delivery across outpatient oncology clinics, inpatient rehabilitation units, and community survivorship programs. Group classes, individual sessions, home-practice materials, and tele-yoga formats have all demonstrated feasibility. The infrastructure for broader implementation exists in many settings.
The barriers, however, are named clearly. Scaling requires trained professionals with genuine oncology expertise. It requires sustainable funding, institutional support, and clear referral pathways. Patients face real obstacles: cost, transportation, treatment-related fatigue, and in some communities, cultural skepticism. Clinicians remain hesitant without standardized protocols and evidence of long-term cost-effectiveness.
These are not peripheral concerns. They represent the field’s next body of work — and they point directly to the role of professional training, advocacy, and interdisciplinary collaboration.
What This Means for yoga4cancer Professionals
The review’s conclusions align closely with the standards the yoga4cancer Method: evidence-informed practice, individualized intervention, trauma-informed teaching, and deep understanding in the realities of cancer treatment and side effects. As healthcare providers increasingly seek credentialed Oncology Yoga practitioners, the value of rigorous, oncology-specific training has never been clearer.
If you are a yoga professional considering this work, or a healthcare provider looking to understand what qualified oncology yoga looks like in practice, the research is pointing in a clear direction.
Venkata Karthik et al. “Integrative Role of Yoga and Naturopathy in Cancer Rehabilitation: A Narrative Review.” Cureus 18(3): e105544. March 2026. DOI: 10.7759/cureus.105544. Review research.



